
It was a little challenging for Midwife Maureen Babine from Iganga Hospital to embark on an unusually early morning trip from Kampala to Kiwoko Hospital in Nakaseke District. She had arrived in Kampala the previous evening from Iganga.
The bumpy drive stretching about 12 kilomeres from Luwero to Kiwoko did not make life any easy for Maureen, who together with other midwives from six hospitals in the Busoga area, were on a learning trip to Kiwoko Hospital, last month.
According to Dr Gertrude Namazzi, the Uganda Manager of the East Africa Preterm Birth Initiative (PTBi) which sponsored the excursion, “the objectives of the trip included learning from Kiwoko’s experiences on what works in terms of set up of their neonatal care unit, how it is managed, and their experiences in monitoring of preterm and sick newborn babies particularly in the area of vital signs observation and feeding, and how they are running their newborn follow up clinic.”
Back to Maureen, upon reaching Kiwoko and listening to their story of twenty years of neonatal care and seeing how things work there, she was amazed and took notes.
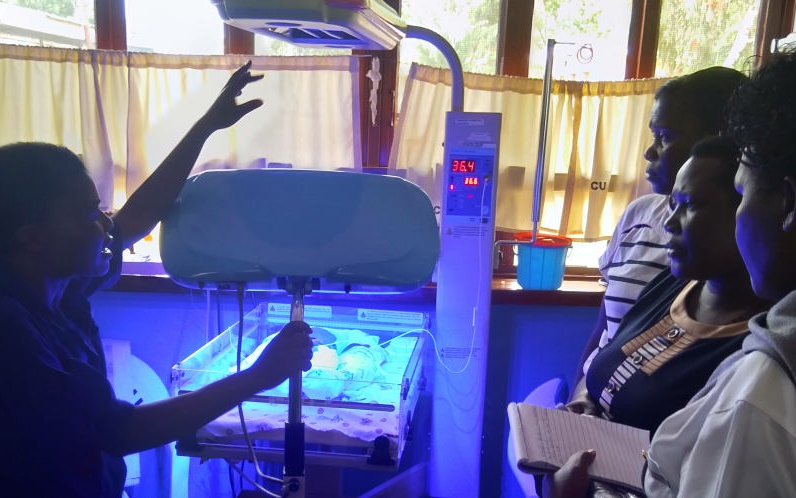
“They have the equipment. They have adequate numbers of midwives and nurses. There are strict infection control measures in place and the space is enough for them. Each baby has their own equipment from a thermometer, stethoscope, to a monitor by their cot. No sharing whatsoever,” Maureen told this writer when sounded out in the aftermath of the visit.
Maureen was so inspired that immediately after returning to her work station, she put into practice two things she had learnt at Kiwoko as she awaits discussions with her superiors on what else can be implemented, of what she picked from Kiwoko.
“We have been giving 2.5 mls of hemo forte whether a baby is preterm or full-term, but they give 0.6mls which is effective for preterm babies. We have changed to this as well. It is commensurate to the age of preterms. They are using syringes which makes it even easy for the mother to learn and even administer the drug,” says Maureen, who heads Iganga Hospital’s Special Care Unit. But this is not the only change she has instituted. She adds: “I remembered that had a monitor which was lying idle somewhere. I went and picked it and we are now using it to monitor babies in our special care unit in the morning and evenings.”
While welcoming the visiting delegation at the time of the excursion, Kiwoko Hospital Medical Director Dr James Nyonyintono said that newborn care at the facility has evolved over the last twenty years. Starting off with two non-functional incubators and three baby cots in a tiny room, in place now is a 36-bed state of the art Newborn Intensive Care Unit.
“A visiting American nurse started us off by teaching us how to resuscitate babies and we got excited when we started saving babies. Since then we have been reading protocols on how to manage newborns and visiting other facilities, pick a few things from what they are doing which we then improve through innovations and perfect it,” Dr Nyonintono told his visitors.
At Kiwoko, training and sharing experiences which sees them conducting two bi-monthly continuous professional development sessions, making use of internationally approved newborn care protocols, infection control, staffing, promoting kangaroo care and effective use of continuous positive airway pressure (CPAP) have been instrumental in their success story.
“We also used to wait for jaundice to show up in preterm babies before we could intervene but nowadays each of them [preterms] get a minimal dose and we have seen a deep in babies who were dying because of jaundice,” Dr Nyonyintono explained, adding that the strict infection control measures in place were informed by the fact that sepsis was the main cause of death among newborns.
None-the-less, the medic emphasised training of key staff and having the knowledge to do what needs to be done to save sick and small newborns. For new staff and those who get to the NICU during internal rotation at the hospital, a two-week orientation before touching any baby is a must and the same rule applies to trainees at the adjacent nursing and midwifery training institution which has been key in supplying manpower to the hospital.
“For instance, as we embrace the use of oxygen, its administration needs skilled personnel. Without the knowledge to administer it, we may end up seeing many cases of blind children who just need a little bit of oxygen but are given more than they need,” said Dr Nyonyintono.
Other noticeable contributory factors to the Kiwoko newborn care success story is the conducive environment for mothers of the sick babies. They are given comfortable accommodation a few metres from the NICU, a comfortable kangaroo care station within the NICU, and restricted access to the NICU.
A Monday to Friday follow-up clinic with clients seen on different days eases the pressure on staff in case the clinic was to be held once a week, a rehabilitation centre for those who may develop developmental defects is also in place.
Currently, premature babies born with weight of less than a kilogramme have an 88 percent chance of survival at Kiwoko. The NICU at the hospital has an average annual admission of 1000 babies both full-term and preterm combined. Regardless of the length of stay, each admission costs 20,000 ($5) Uganda Shillings, thanks to the shot in the arm from the charity ADARA Group, whose aim is to work side by side with women, children and their communities in remote and rural areas such as Kiwoko.

